If you or your loved one has been diagnosed with midshaft femur non-union, you may be concerned about delayed healing, mobility limitations, and the possibility of further surgery. At our orthotic clinic, we specialize in evidence-based orthotic management for femoral shaft fractures, helping patients regain stability, confidence, and functional independence.
One effective approach for managing midshaft femur non-union is the use of a Femoral Functional Fracture Brace, which provides necessary support and promotes healing.
In this case-based educational blog, we discuss the condition, radiological findings, and the advanced orthotic solution provided to a 21-year-old female patient with femoral shaft non-union and callus formation.
What is Midshaft Femur Non-Union?
The femur (thigh bone) is the longest and strongest bone in the body. A fracture in the midshaft region can occur due to trauma, accidents, or high-impact injuries.
Non-union occurs when the fracture fails to heal within the expected timeframe (typically 6–9 months). Instead of forming solid bone bridging across the fracture site, healing remains incomplete.
Common Causes of Femoral Non-Union
- Inadequate fracture stabilization
- Excessive micromotion
- Poor alignment
- Infection
- Biological healing imbalance
- Premature weight-bearing
In young adults, especially females with good bone biology, non-union often results from mechanical instability rather than poor healing potential.
Radiological Features of Femoral Shaft Non-Union
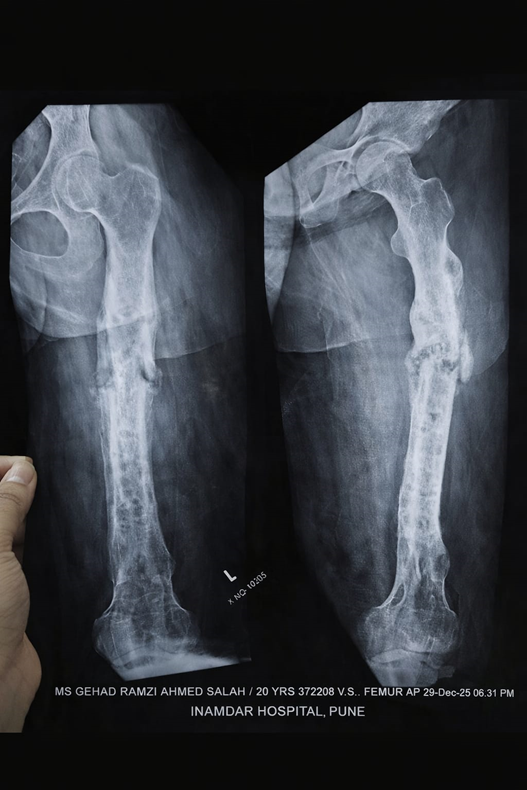
In this 21-year-old patient, the X-ray findings showed:
- Persistent fracture line at midshaft
- Significant callus formation
- Cortical irregularity
- No complete bridging union
The presence of callus indicates that the body is attempting to heal — a positive sign. This type of pattern is often described as hypertrophic non-union, meaning biology is good but stability is insufficient.
Why Functional Bracing is Effective in Hypertrophic Non-Union
Sarmento Principle of Functional Fracture Bracing
The Sarmento principle, developed by Augusto Sarmiento, is based on the concept of functional fracture bracing, where controlled motion and early weight-bearing are encouraged to promote natural bone healing.
Key Points of the Sarmento Principle:
- Early Mobilization – Instead of prolonged rigid immobilization, joints near the fracture are allowed to move.
- Controlled Compression – Muscle contraction during movement creates gentle circumferential compression at the fracture site.
- Functional Loading – Partial weight bearing stimulates callus formation and enhances bone healing.
- Soft Tissue Support – A well-fitted functional brace stabilizes the fracture through soft tissue containment rather than rigid fixation.
- Improved Healing Environment – Micromovements promote biological healing and reduce complications like joint stiffness and muscle atrophy.
The Sarmento principle believes that movement and controlled loading help bones heal better than complete immobilization, provided the fracture is properly aligned and supported with a functional brace.
When biological healing potential is present, the main goal is to improve mechanical stability. That is where a Femoral Functional Fracture Brace becomes highly effective.
Key Benefits of Femoral Functional Fracture Brace
- Circumferential compression of soft tissues
- Improved fracture alignment
- Load-sharing during weight-bearing
- Reduced abnormal rotational forces
- Promotion of secondary bone healing
- Prevention of muscle wasting
Functional bracing follows the principle that controlled compression and micromotion stimulate bone healing.
Advanced Orthotic Solution: Femoral Functional Fracture Brace + TES Belt (AK)

One of the most common issues with femoral braces is downward migration (slipping) during walking. This can reduce compression and compromise fracture stability.
To overcome this, we provided:
✔ Femoral Functional Fracture Brace
✔ TES Belt (Above Knee) Suspension System
What is an TES Belt (AK)?
The TES (Total Elastic Suspension) Belt Above Knee system enhances:
- Proximal suspension
- Anti-slip control
- Uniform compression maintenance
- Rotational stability
- Patient comfort during ambulation
In young female patients, thigh shape and soft tissue contour may contribute to brace migration. The AK suspension ensures the brace remains securely positioned, especially during weight-bearing activities.
Biomechanical Principles Behind the Treatment
1. Hydrostatic Compression
Soft tissue compression distributes pressure evenly around the femur.
2. Load Sharing
Encourages natural bone remodelling under controlled weight-bearing.
3. Controlled Micromotion
Promotes callus maturation and secondary bone healing.
4. Muscle Containment
Reduces deforming forces caused by muscle contraction.
These principles work together to create an optimal healing environment.
Orthotic Management Protocol at Our Clinic
Initial Assessment
- Detailed clinical evaluation
- Gait analysis
- Pain scoring
- Muscle strength assessment
- Radiographic review
Custom Fabrication
- Accurate limb measurement / Casting
- Thermoplastic shell fabrication
- Soft interface lining
- Adjustable compression straps
- TES Belt integration
- Holes are provided for better breathability and ventilation.
Why Early Controlled Weight-Bearing is Important
Research supports that controlled loading:
- Stimulates osteogenesis
- Improves callus consolidation
- Enhances bone remodelling
- Reduces risk of further non-union
In young patients, this approach can significantly improve healing timelines.
Expected Outcomes of Orthotic Treatment
With proper compliance and multidisciplinary care, patients can expect:
- Improved fracture stability
- Prevention of deformity
- Enhanced healing potential
- Reduced risk of surgical intervention
- Return to functional mobility
For a 21-year-old female, this approach also supports long-term bone health and active lifestyle recovery.
When to Consider Functional Bracing?
Functional femoral bracing is ideal when:
- Callus formation is present
- No active infection exists
- Alignment is acceptable
- Surgery is not immediately indicated
- Patient compliance is good
Early orthotic intervention can prevent prolonged disability.
Final Thoughts
Midshaft femur non-union can be challenging, especially in young patients eager to resume normal activities. However, when biological healing potential exists, Femoral Functional Fracture Bracing combined with TES Belt (AK) suspension offers a powerful, non-surgical pathway toward recovery.
Through advanced orthotic care, controlled compression, and guided rehabilitation, we help patients regain confidence, stability, and mobility.








